Missing teeth do more than just impact your smile. They can affect how you chew, speak, and even how comfortable you feel in social situations. Many adults are also concerned about the possibility of long-term bone loss after losing teeth. That concern makes sense. Nobody wants to invest time in treatment and later deal with pain or complications. People enjoying summer events or grabbing dinner along the bayfront often want a solution that feels natural and stable for daily life. Dental health becomes part of confidence, comfort, and routine activities.
The good news is that true rejection remains uncommon. Most implants succeed when patients receive proper planning and ongoing care. However, in certain situations, the surrounding tissue may not heal properly or fail to bond with the jawbone. At Harborcreek Dental, patients receive personalized guidance and modern restorative care designed to support long-term oral health. Understanding the risks, symptoms, and prevention steps helps patients make informed decisions before treatment begins.
What Really Happens During the Treatment Failure?
Dental restorations are a great, durable option for replacing missing teeth, but it’s natural to ask: Can dental implants be rejected? So find out what really happens during the failure:
The Body Usually Accepts Titanium Well
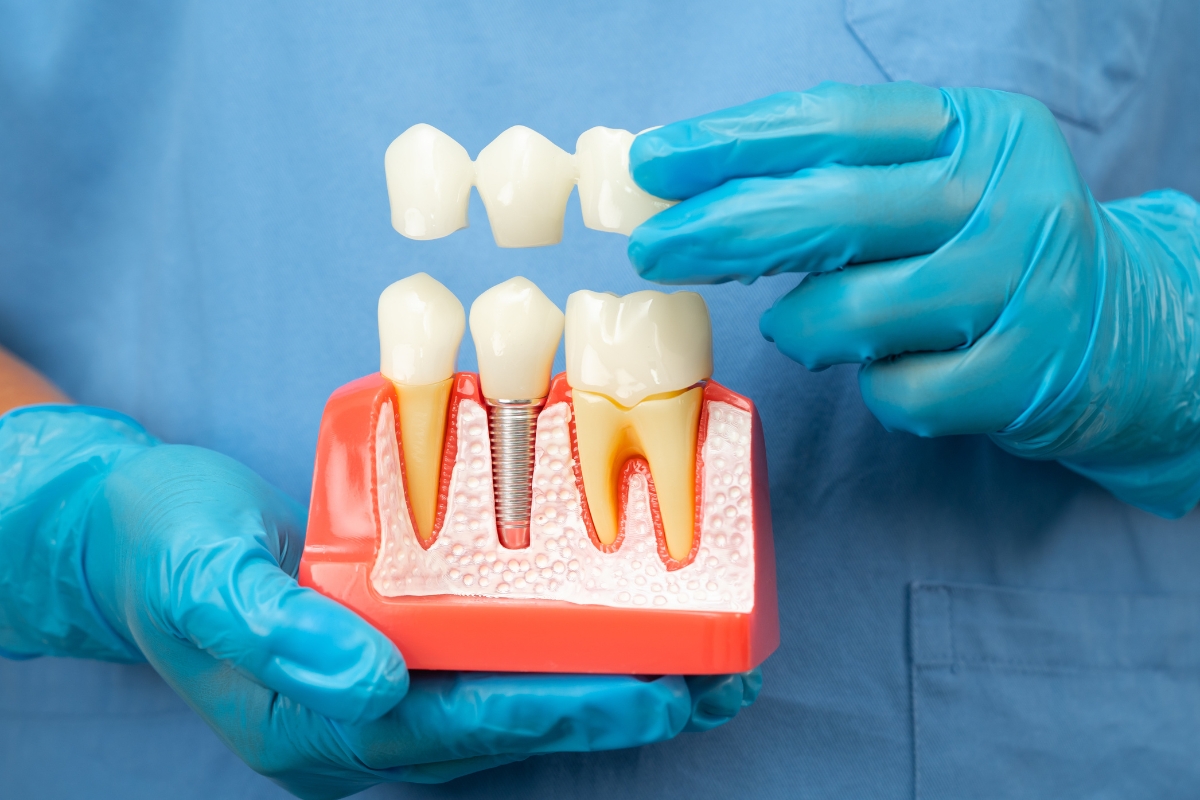
Prosthetic teeth commonly use titanium because the material works well with human bone. After placement, the jaw gradually bonds with the fixture through a process called osseointegration. This connection helps create stability for chewing and speaking. The American Academy of Implant Dentistry reports success rates above 95 percent in healthy patients. That number shows how predictable treatment has become when proper planning occurs.
Failure Often Comes From Healing Problems
Many patients assume the immune system attacks the fixture directly. In reality, most complications involve infection, poor healing, or pressure on the surgical site. Gum disease and smoking also increase complications. The restoration may loosen if the bone does not fuse correctly. Some patients notice discomfort during chewing or swelling around the gums. These issues need attention before damage worsens.
Timing Matters During Recovery
Some complications appear early during healing. Others develop years later because of bone loss or bacterial buildup. Patients who skip follow-up visits often miss the early warning signs. After winter lake effect snowstorms, many residents delay routine oral care visits, which can allow inflammation around restorations to worsen unnoticed.
Why Do Some Dental Restorations Struggle to Heal Properly?
If you are wondering, “Why do dental implants fail?”, you need to understand why some people struggle in the first place. Here are the reasons:
Existing Oral Health Problems Create Risk
Healthy gums support long-term stability. An active gum infection weakens surrounding tissue and increases bacterial growth around the surgical area. Patients with untreated periodontal concerns may face a greater chance of complications. Bone density also matters because they require strong support beneath the gums.
Smoking Slows Healing
Nicotine reduces blood flow and slows recovery. Healing tissue receives less oxygen, which affects the bone bonding process. Smokers often experience delayed healing and higher failure rates. This does not automatically prevent treatment. However, patients benefit from discussing lifestyle habits before surgery begins.
Certain Medical Conditions Affect Recovery
Conditions like uncontrolled diabetes may interfere with healing. Some medications also affect bone metabolism. Thorough health reviews help providers plan safer treatment approaches. According to the National Institute of Dental and Craniofacial Research, oral inflammation can influence overall health and healing outcomes.
Poor Bite Pressure Can Damage Restorations
Grinding or clenching creates repeated stress on the surgical site. Excess force may weaken the surrounding bone over time. Patients who experience nighttime grinding may require protective treatment options to reduce pressure during sleep.
Signs Your Implant May Need Professional Attention
These are the symptoms that indicate that you need professional care:
Persistent Pain Is Not Normal
Mild soreness after placement is expected for a short period. Ongoing discomfort weeks later deserves evaluation. Sharp pain during chewing often signals a deeper problem. Ignoring pain may allow bone deterioration to continue unnoticed.
Swelling and Gum Changes Need Monitoring
Redness, swelling, or bleeding around the surgical area may indicate infection. Healthy tissue should look firm and pink after recovery finishes. Patients sometimes notice a bad taste or odor near the site. That symptom may point toward bacterial buildup beneath the gums.
Loose Movement Requires Immediate Care
A prosthetic tooth should feel stable. Movement or shifting often means the bone connection has weakened. This issue rarely improves without treatment. Quick evaluation helps preserve surrounding tissue and reduce further complications.
What Happens if an Implant Stops Functioning Correctly?
There are steps to take and options available to keep everything on track. Here they are:
The Area Requires a Detailed Evaluation
Patients often panic after hearing treatment failed, but modern dentistry offers ways to address complications. The first step involves identifying the cause by examining bone levels, gum health, and bite alignment. This stage becomes important when discussing what happens if a dental implant fails because treatment depends entirely on the underlying issue. Patients considering long-term solutions with implant dentistry solutions in Erie, should understand that proper diagnosis and treatment planning play a major role in long-term success.
Infection Control Comes First
If bacteria caused inflammation, the surrounding tissue must heal before additional treatment begins. Deep cleaning around the surgical area may help control infection. Some cases require removing damaged tissue to protect nearby bone.
Implant Replacement May Still Be Possible
Patients often assume failure means those restorations can never work again. That belief remains inaccurate in many situations. Once healing improves, another prosthetic tooth may still succeed.
Bone Support Sometimes Needs Improvement
Bone loss near the surgical area might need some rebuilding before we can put in another restoration. Taking the time for careful treatment planning really helps ensure better stability down the road.
How Can Patients Protect Tooth Restorations for the Long Run?
Here are the tips you need to follow:
- Consistent Home Care Matters Daily: Those restorations require daily brushing and flossing just like natural teeth. Bacteria still affect the gums surrounding the structure.
- Routine Visits Catch Problems Early: Professional monitoring helps identify issues before major damage develops. Small gum changes often appear before patients notice symptoms themselves.
- Choosing the Right Treatment Planning Makes a Difference: Every mouth heals differently. Thorough evaluations help determine whether the jawbone, gums, and overall health support successful treatment.
- Lifestyle Choices Influence Longevity: Healthy habits support better healing. Balanced nutrition, reduced tobacco use, and stress management all contribute to stronger recovery.
There are several approaches for how dentists fix failed implants, depending on the cause of the problem. However, prevention and early care remain the best ways to protect long-term success.
Restore Your Missing Teeth with Our Professional Care
Dental implants continue to help many adults restore their smiles successfully. While complications can occur, true rejection remains uncommon. Most problems develop from infection, healing challenges, or excessive pressure around the surgical area. Understanding symptoms early gives patients a better chance of protecting their oral health. Delaying care often allows inflammation and bone damage to progress further.
At Harborcreek Dental, our team provides restorative care designed to help patients regain comfort, stability, and confidence after tooth loss. If you are experiencing discomfort, loose restorations, or concerns about healing, schedule an appointment to explore treatment options tailored to your smile goals.
FAQs
Yes, late complications sometimes occur because of gum infection, bone loss, or excessive bite pressure. Problems may develop gradually, which makes regular monitoring important for protecting surrounding tissue and maintaining long-term stability.
Strong bone support helps stabilize the restoration after placement. Patients with reduced bone density may require additional evaluation before treatment to improve healing and create better support for long-term function.
Yes, grinding places repeated force on the prosthetic teeth and surrounding bone. Long-term pressure may weaken stability or damage restorations if patients do not manage nighttime clenching habits properly.
Healing varies between patients, but many people require several months for complete bone integration. Gum health, overall wellness, and lifestyle habits all influence recovery speed and long-term outcomes.
Yes, bacteria may collect around the surgical area and inflame nearby tissue. Without treatment, the infection can damage bone support and threaten the stability of the restoration over time.
Not always. Some patients notice subtle swelling, bleeding, or looseness before pain begins. Routine examinations often identify early warning signs before major discomfort develops or additional treatment becomes necessary.

